Key Takeaways
- Lipedema is a chronic fat disorder that is not the same as mere “stubborn fat” because it features different cellularity, inflammation, and often causes pain and irregular fat distribution, particularly in the limbs.
- Unlike ‘stubborn fat’, lipedema does not respond to typical weight loss strategies, making personalized treatment and early diagnosis essential for effective management.
- Hormonal shifts during times like puberty, pregnancy, or menopause and heredity can all put you at a greater risk for lipedema, so it’s important to be aware of your family history.
- A proper diagnosis is based on clinical evaluation, patient history, and sophisticated imaging that differentiate lipedema from other fat-related conditions.
- There is an emotional toll that comes with living with lipedema. Body image battles and the frustration of constantly being misdiagnosed make mental health support and community resources invaluable.
- Managing lipedema can involve both conservative care, like anti-inflammatory diets and compression therapy, and surgery. Research continues on how to help those affected.
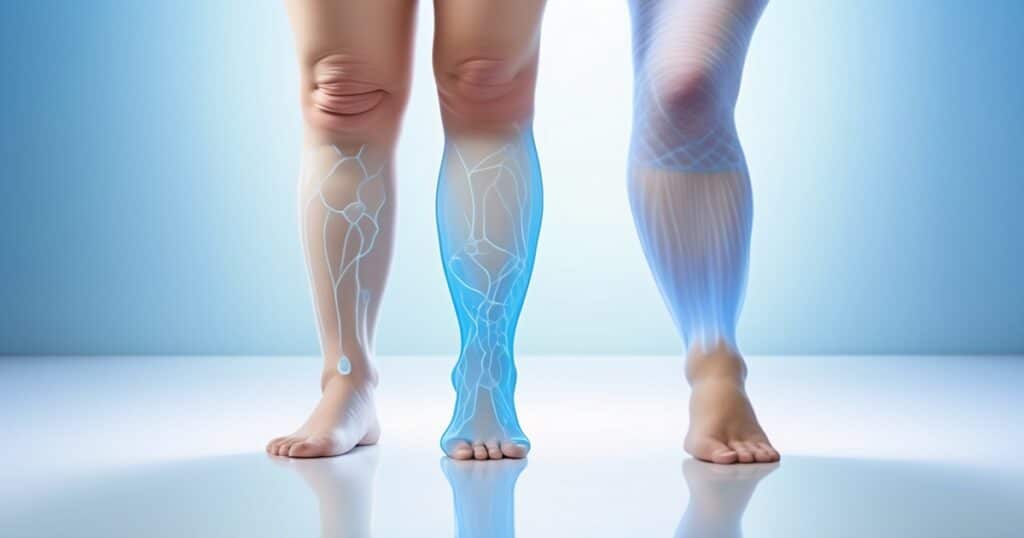
Lipedema is a medical condition that results in fat deposits in the legs and arms.
Stubborn fat” typically refers to areas of body fat that resist reduction despite diet and exercise.
They each require a different approach to treat and manage.
To help clarify the key distinctions, the following sections discuss symptoms, causes, and treatment measures for each disorder.
The Core Distinction
Lipedema and “stubborn fat” can appear similar at first glance. They behave, look, and respond to treatment differently. Lipedema is a fat tissue disorder, not just excess fat due to weight gain. It predominantly impacts the legs and is characterized by pain, edema, and weight loss resistance. Knowing these differences is crucial to good care and better living.
1. Cellular Nature
Lipedema fat cells are not ordinary fat cells. They tend to be bigger, more likely to bulge and harder to digest. This fat tissue contains more fluid and is prone to low-grade inflammation that can make it tender and sore.
Regular adipocytes react to diet or exercise, decreasing in size as the body expends stored calories. Lipedema cells don’t shrink as easily, no matter how much you diet or work out.
Fibrosis, or tissue thickening, is prevalent in lipedema. This causes the fat to feel denser, occasionally lumpy, and less responsive to non-invasive interventions. Fibrosis implies the tissue can be ropey-feeling, which is not normal for regular fat.
2. Body Symmetry
Those with lipedema commonly observe an obvious body shape mismatch. The bottom half, including the legs, buttocks, and occasionally arms, becomes vastly bigger than the top half, while feet are untouched.
Standard fat gain is more balanced, with pounds accumulating in the abdomen, back, arms, and legs. The shape shifts from lipedema can make clothing fit funny and impact body image.
This asymmetrical fluff can drag down motion and potentially stress joints. In time, it can impact how you walk, stand or perform daily activities.
3. Physical Sensation
Pain is an enormous difference. Lipedema fat bruises to the touch and feels weighty or sore, particularly following extended intervals of standing. The vast majority of stubborn fat holders experience no pain in those regions.
Swelling is another hint; lipedema swelling doesn’t resolve with rest, as swelling from standing too long does. A few will have lymphedema too, for added pain, tightness, and skin changes.
4. Skin Texture
Skin above lipedema fat tends to be soft, bumpy and irregular, like cottage cheese. Normal fat is softer and less prone to dimpling unless cellulite exists.
The existence of these thickened folds or nodules indicates lipedema and is employed by physicians to aid in diagnosis. Feeling skin texture is an easy but crucial test in differentiating these conditions.
5. Lifestyle Response
Lipedema is tenacious. Diet and exercise scarcely reduce the involved fat. Millions of lipedema patients eat well and exercise, yet nothing shifts.
Hormones might be involved, as lipedema frequently begins or exacerbates at puberty, pregnancy, or menopause. Since conventional weight-loss programs fall flat, physicians propose personalized strategies such as compression therapy, light exercise, and occasionally surgery.
Underlying Causes
Lipedema and stubborn fat have distinct underlying causes, and understanding these aids in effective treatment. Lipedema is a long-term disease that causes abnormal fat deposits, primarily in the legs and arms. This condition tends to appear during life periods that involve significant hormonal shifts, such as puberty, pregnancy, or menopause.
Unlike stubborn fat, which typically stems from lifestyle or metabolic factors, lipedema possesses distinct triggers and patterns. Symptoms such as pain, easy bruising, and symmetrical fat accumulation may be misattributed to other problems, such as obesity or lymphedema.
Hormonal Triggers
Hormones are a huge factor in the onset and worsening of lipedema. Estrogen is most notable, as a lot of cases begin or flare when estrogen fluctuates, which is why lipedema commonly presents in the teen years, pregnancy, or during menopause. Hormonal therapies, which seek to balance or alter these hormone levels, can assist in managing lipedema for some. However, outcomes vary individually.
- Estrogen surges during puberty
- Hormonal shifts in pregnancy
- Menopause-related hormone drops
- Use of hormonal birth control
- Insulin resistance
- Excess cortisol from chronic stress
Insulin resistance is another culprit. It can cause abnormal fat storage that exacerbates lipedema. Other studies implicate the fat cells themselves in lipedema. These cells become hypertrophic and act differently than normal fat cells.
They do not react well to calorie restriction or exercise. This special fat, encased in a geloid matrix with hyaluronic acid and water, might be why conventional weight loss approaches seldom prove effective against lipedema.
Genetic Links
Lipedema runs in families, demonstrating a strong genetic connection. Many individuals with lipedema note that their mother, sisters, or daughters had similar symptoms. Research from Europe and beyond points to certain genetic markers as increasing the risk, but the overall outline remains incomplete.
This hereditary nature allows for early diagnosis if there is a family history. Awareness of familial connections is important as it aids in detecting lipedema in its early stages, sometimes ahead of noticeable symptoms.
Genetics proves that lipedema fat isn’t your average stubborn fat. The tissue is hypertrophic and grows way beyond the ordinary, sometimes in both legs and arms simultaneously. This pattern is distinct from typical fat accumulation that is not associated with a genetic history.
Doctors can use a patient’s family background as a simple but powerful tool to assess risk. It helps rule out other conditions that look similar but have different causes, like obesity or lymphedema.
Diagnostic Journey
Diagnosing lipedema is not always straightforward. It usually begins when a reasonably healthy person observes changes in their body that don’t align with typical fat gain. Millions more suffer for years from mysterious swelling, pain, or changes in their legs and arms. They can be told they just have ‘stubborn fat’ or that their symptoms are lifestyle-related, which are dismissive and frustrating diagnoses.
True lipedema fat is not the same as regular fat. It’s usually symmetrical, impacting both legs or arms, and doesn’t react to diet or exercise in the same manner. That results in recurring weight loss efforts, clinic-hopping, and occasionally overtreatment.
Clinical Evaluation
A clinical evaluation is the initial, significant step. Physicians look for tell-tale signs, such as swelling that isn’t resolved by rest and fat that is soft, lumpy, and tender. They check for easy bruising, which is prevalent in lipedema, and inquire about pain, heaviness, and the impact on daily life.
Fat distribution is key. Lipedema fat tends to spare the hands and feet, whereas more classic stubborn fat from other causes typically does not have that defined border. An attentive history is equally important. Doctors need to hear when your symptoms began, if they fluctuate with hormones, and if there is a family history of similar issues.
This helps differentiate lipedema from obesity or lymphedema, which may appear alike but differ in pathogenesis and management. A good diagnostic journey is a process, and it may take years, but it provides the patient with the crucial feeling of being listened to.
Most doctors are not trained to identify lipedema. Patients often see several clinicians. Others are misdiagnosed with lymphedema or venous disease or told it’s because they’re living poorly. This delay can cause more pain and sometimes disability.
A complete approach means not just looking at physical signs, but asking about pain, quality of life, and mental health. Lipedema can affect daily activities and emotional wellbeing, so a good evaluation covers all these bases.
Imaging Techniques
Imaging aids in making the diagnosis and excluding other etiology. Ultrasound is most commonly used initially. It may be able to differentiate between lipedema fat and regular fat by demonstrating alterations in tissue architecture.
MRI scans provide even more detail, charting the thickness and spread of involved fat and assisting in identifying fluid collections or other complications.
| Technique | Use Case | Strengths | Limitations |
|---|---|---|---|
| Ultrasound | Tissue structure | Quick, widely available | Operator dependent |
| MRI | Fat mapping, severity | High detail, no radiation | Cost, access |
Imaging is helpful not only in diagnosis but in treatment planning. Doctors can monitor trends, observe disease progression velocity, and tailor treatments accordingly. For patients, this translates into reduced trial and error and increased precision treatment.
Digital imaging provides both patients and physicians with definitive visual evidence that lipedema is real and distinct from standard fat. This can be affirming after years of uncertainty.
Specialized lipedema providers are key. They know the nuances and they know which tests count. They can link patients to support and provide newer treatments GPs might not discuss. Having an expert along for the journey can abbreviate the lengthy road to diagnosis and improved treatment.
The Emotional Toll
There’s an emotional toll that comes with living with lipedema. Everyday pain, swelling, and dramatic changes in body shape can make basic routines difficult. A lot of lipedema women feel dismissed or neglected, which exacerbates the frustration or isolation. Chronic pain, heaviness, and swelling tend to erode self-esteem.
Anxiety and depression aren’t uncommon, particularly when diagnosis is delayed. Without the appropriate support, mental health can suffer and the feeling of control over one’s own body evaporates.
Misdiagnosis Impact
Mistaking lipedema for plain old obesity or “stubborn fat” can lead to a domino effect of issues. Folks can hear unhelpful diet or exercise advice, which can cause guilt, shame, or blame-the-victim feelings. This misconception can cause treatment plans that miss the true problem, occasionally exacerbating symptoms.
For instance, others might spur themselves with intense workouts to find more swelling and pain. Others attempt hardcore diets and still experience zero difference in problem spots. This cycle wears you down.
Getting brushed off by doctors or not being taken seriously is another huge component of the emotional cost. Many patients recount experiences of being talked over or blamed for their symptoms. It can take some years to receive the right diagnosis.
This is when the emotional toll starts to accumulate. They may quit looking for help, believing nobody will hear them or care. Unawareness among doctors is a primary obstacle. More education and more guidance can prevent these bad experiences in the first place.
Body Image
Lipedema alters the perception of their body. There’s swelling in the legs, hips, or arms which pops out and rarely agrees with the rest of the suit. This frequently invites unsolicited remarks, which not only sting but bolster self-doubt.
Social norms and beauty ideals exacerbate the situation, particularly when the media emphasizes slenderness or particular body types. Lipedema patients often feel like misfits, which results in diminished confidence or depression.
It’s not easy to build a better body image. Support groups or online communities provide room to swap stories, trade strategies, and cheer on little victories. Small moves, such as centering on what the body can do versus how it appears, can strengthen resilience.
Mental health care, whether that involves sessions with a counselor or joining a support group, can lighten the burden. Support of family and friends counts as well. Acceptance increases when individuals experience the sensation of being observed, listened to, and appreciated as more than their illness.
Management Approaches
Management for lipedema and so-called ‘stubborn fat’ differs because of the origins and manifestations. Management approaches for lipedema, a chronic condition with distinctive fat cell biology, differ from stubborn fat, which consists of localized fat deposits that do not easily respond to traditional weight loss efforts.
Both need distinct care plans, and strategies can consist of lifestyle modifications, conservative treatments, and occasionally surgery. Effective lipedema care often requires a multidisciplinary approach that targets symptoms such as pain, swelling, and bruising, as well as aesthetics.
Conservative Care
| Option | Description | Benefits |
|---|---|---|
| Compression Therapy | Wearing special garments to reduce swelling and discomfort | Eases pain, controls swelling, supports daily function |
| Manual Lymphatic Drainage | Gentle massage technique to help lymph flow | May lessen swelling, improve comfort |
| Physical Therapy | Movement and exercise plans tailored to the individual | Improves mobility, reduces pain, maintains limb health |
| Nutritional Support | Guidance from dietitians on anti-inflammatory diets | Promotes overall health, may ease symptoms |
| Skin Care | Moisturizing and gentle skin handling | Reduces risk of infection, keeps skin healthy |
Lifestyle changes such as an anti-inflammatory diet can contribute to symptom relief by reducing inflammation and swelling. For example, some add more whole foods, fish, and nuts to the mix while reducing processed foods and sugars.
Diet and exercise alone don’t usually make a difference to lipedema fat, but they are still crucially important to your overall health and preventing symptoms from progressing. Nutritional support is another focus of care. Dietitians might suggest foods that aid the lymph system and control weight.
Even if the weight loss is minimal, these steps can still increase energy and well-being. You need regular check-ins and plan adjustments. Lipedema can evolve, meaning continuous follow-up helps keep symptoms under control.
Maintenance is important as lipedema and cellulite can be chronic and require ongoing attention.
Surgical Options
- Reduces excess fat in targeted areas
- Can improve pain, mobility, and appearance
- Possible risks: infection, nerve damage, scarring
- Surgery does not cure lipedema but may ease symptoms
- Requires careful aftercare and follow-up
Surgery, like liposuction using specialized techniques, can remove diseased fat and might reduce pain and swelling. Most experience better outcomes than with conservative care alone.
This can translate into improved mobility and an improved quality of life. Still, it’s not a cure and symptoms can come back if left untreated. Risks are tangible. Any surgery has the risk of infection or scarring.
Others could have nerve damage or slow healing. Selecting an experienced lipedema surgeon is essential to ensure safety and optimal results. Non-invasive alternatives like ultrasound or radiofrequency can assist in cellulite management through enhanced skin texture.
These can be incorporated into an overall strategy and are less effective for actual lipedema.
Beyond The Diagnosis
It’s not just about the diagnosis of lipedema. A lot of people are just relieved to know what’s causing their pain and swelling. Having answers enables them to process years of symptoms and transformations in their body. The obstacles don’t stop there. Lipedema can make daily life painful.
It might cause pain, torment, and soul-shattering tension. A few of these struggle to get around or keep up with work. Some become depressed, stressed, or begin to lose confidence. Patients often feel like they’re being dismissed, particularly when doctors don’t even know about lipedema. This hesitation towards seeking assistance can make it more difficult to manage.
Continuous education about lipedema is important for patients and medical professionals alike. When more are aware of the symptoms, it becomes easier to differentiate between lipedema and what some refer to as ‘stubborn fat.’ Workshops, online courses, and trusted sources can assist.
By sharing stories and facts about lipedema on social media, you’re potentially reaching people who had no idea such a condition even existed. The more doctors and nurses learn, the more patients receive the right care early.
Support groups and communities mean a whole lot for lipedema warriors. Meeting others who are struggling with the same things is comforting. In-person groups, online forums, and social media pages provide a space to exchange advice and experiences.
They trade tips on what works, like massage or easy home treatments. They can help handle the hard emotions that accompany the diagnosis. When they feel less alone, they’re more likely to persevere with their care plan and discover hope.
Advocacy is required to drive research and improved treatment options. So many countries still have so little resources for lipedema. These are the organizations that can help by demanding increased funding for research and expanding access to treatments.
They advocate for lipedema to be more recognized in media and health discussions. This will help lead to better therapies, insurance coverage, and fair treatment for those who live with it.
It’s important to have open discussion between patient and doctor. It makes care more human and efficacious. Patients should feel comfortable disclosing all symptoms, even the minor ones.
A doctor needs to listen, ask questions, and hear the full impact on daily life. Small adjustments, such as extended visits or return phone calls, can have a huge impact.
Conclusion
Lipedema and “stubborn fat” both alter the way people look and feel, but have very different causes and solutions. Lipedema presents with pain, swelling, and thick legs or arms, whereas stubborn fat generally remains even after dieting or exercising. A lot of people confuse the two and end up wasting time or money on fixes that don’t work for lipedema. Knowing the signs can help someone find care that fits. Those of us with lipedema deserve real answers, not blame or shame. To get assistance, consult a fat disorders-aware physician. Request information, seek assistance, and advocate for yourself. Facts paved the way to my health and my life.
Frequently Asked Questions
What is the main difference between lipedema and stubborn fat?
Lipedema is a progressive disease that results in the buildup of excess fat, mostly in the legs and arms. Stubborn fat is normal fat that doesn’t respond to diet or exercise easily. It’s not due to a medical condition.
Can lipedema be reduced with diet and exercise?
No, lipedema fat does not respond to diet or exercise. Healthy habits do wonders for overall health, but lipedema typically requires targeted medical intervention to reduce its severity.
How is lipedema diagnosed?
Lipedema is diagnosed by a healthcare provider through physical examination, patient history, and occasionally imaging tests. Early diagnosis is key, so if you see consistent, symmetric swelling in your limbs, see a qualified professional.
What causes lipedema?
We don’t know the exact cause of lipedema. It tends to be hereditary and can be associated with hormonal shifts, like puberty, pregnancy, or menopause.
Is lipedema painful?
Indeed, many lipedema patients experience pain, tenderness, or easy bruising in impacted areas. Stubborn fat typically does not hurt.
Can lipedema affect mental health?
Yes, lipedema may affect mental health. These physical symptoms and appearance shifts can cause stress, low self-esteem or anxiety.
What are the treatment options for lipedema?
Lipedema treatment can encompass compression therapy, manual lymphatic drainage, exercise and in certain instances, specialized surgical interventions such as liposuction. Work with a healthcare provider to develop a treatment plan that’s right for you.

